G UANG -Y I W ANG & S HUI -X ING Z HANG , H ONG -J UN L IU , C HANG -H ONG L IANG , B IAO H UANG
ORIGINAL ARTICLE
Background: Lesion-to-brain contrast after gadolinium administration is signifi cantly higher at 3.0 Tesla (T) compared to 1.5T. The high in vivo relaxivity of gadobenate dimeglumine (Gd-BOPTA) may permit the use of lower-dose contrast agents.
Purpose: To investigate whether low-dose contrast-enhanced MRI at 3.0T using a high-relaxivity contrast agent (Gd-BOPTA) can achieve a comparable or improved contrast-to-noise ratio (CNR) for the detection of brain metastases compared with exami-nation of the same patient at 1.5T using a standard dose of gadopentetate dimeglumine (Gd-DTPA).
Material and Methods: A total of 18 patients with known brain metastases were fi rst imaged at 1.5T with 0.1 mmol/kg Gd-DTPA. Patients returned at least 24 hours later for imaging at 3.0T with Gd-BOPTA at cumulative doses of 0.025 mmol/kg, 0.05 mmol/kg, 0.075 mmol/kg, and 0.1 mmol/kg (0.1 mmol/kg body weight overall). The CNR of enhancing brain lesions compared to the normal contralateral white matter was calculated. For the 3.0T study using different cumulative doses of Gd-BOPTA, the CNR of lesions was compared with CNR of the same lesions imaged at 1.5T using 0.1 mmol/kg Gd-DTPA, by using the Wilcoxon matched-pairs signed-rank test.
Results: At 1.5T with 0.1 mmol/kg Gd-DTPA, the mean CNR between enhanced lesions and cerebral white matter was 12.01 ± 2.53. With 3.0T imaging using different cumulative doses of Gd-BOPTA, the mean CNRs were 7.19 ± 4.06, 15.31 ± 6.37, 25.44 ± 11.02, and 31.88 ± 13.21. At 3.0T with 0.05 mmol/kg Gd-BOPTA, CNR was 1.34-fold higher compared to CNR at 1.5T with 0.1 mmol/kg Gd-DTPA (P <0.01).
Conclusion: Comparable contrast enhancement of brain metastases can be achieved with a 0.05-mmol/kg dose of Gd-BOPTA at 3.0T compared to imaging at 1.5T using 0.1 mmol/kg Gd-DTPA.
Key words: Comparative study; detection; magnetic resonance imaging; metastasis
Biao Huang, Department of Radiology, Guangdong General Hospital, Guangdong Academy of Medical Sciences, Guangzhou, Guangdong, China; #106 Zhongshan 2nd Road, Guangzhou, Guangdong, China, 510080 (fax. +86 20 83870125, e-mail. cjr.huangbiao@ vip.163.com)
Submitted April 14, 2009; accepted for publication September 4, 2009
In patients with known or clinically suspected brain metastases, gadolinium-based contrast-enhanced mag-netic resonance imaging (MRI) is accepted as the most sensitive method of detection. The standard dose of contrast for 1.5T MR imaging systems is 0.1 mmol/kg body weight (1, 2). It has been shown that greater sensitivity can be achieved when higher doses, up to 0.3 mmol/kg gadolinium, are administered (3–5). However, the use of a higher dose of contrast medium not only increases the potential side effects, but also represents a substantial increase in cost, compared to a standard 0.1 mmol/kg dose.
The number of 3.0T systems in clinical settings has been increasing in recent years. One major advantage of high-fi eld imaging is improvement in the signal-to-noise ratio (SNR) compared with 1.5T imaging (6). The increased SNR leads to a higher contrast-to-noise ratio (CNR) between enhancing and non-enhancing tissues. In addition, with the longer baseline relaxation times brought about by the higher magnetic fi eld strength, the T1-shortening effect of Gd-based contrast agents should be greater and the contrast enhancement of the lesions on T1-weighted images should generally be stronger at 3.0T than they are at 1.5T (7). Thus, one can expect that MRI at 3.0T can offer better lesion contrast enhancement and improved CNRs even with a lower dose of contrast agent.
In recent years, gadobenate dimeglumine (Gd-BOPTA, MultiHance; Bracco Imaging, Milan, Italy), which was initially designed for liver imaging, has become available for central nervous system (CNS) imaging. It has a substantially higher T1 relaxivity in blood due to its capacity for weak, transient interaction with serum pro-teins, principally albumin (8, 9). It has been reported in a prospective study (10) that the use of doses lower than 0.1 mmol/kg of GD-BOPTA at 1.5T is suffi cient for the detection of brain metastases. It is unclear to what extent the high-relaxivity contrast agents impact the diagnostic benefi ts at 3.0T. The purpose of this study was to inves-tigate whether a low dose of a high-relaxivity contrast agent (Gd-BOPTA) at 3.0T could achieve comparable or possibly improved CNR of brain metastases compared with a 1.5T examination in the same patient using 0.1 mmol/kg of gadopentetate dimeglumine (Gd-DTPA).
Material and Methods
Our study received institutional review board approval prior to implementation. Informed consent was obtained from all patients. From June 2007 to April 2008, patients with malignant tumors outside the CNS underwent MRI examinations to detect brain metas-tases using a 1.5T system with a standard dose of 0.1 mmol/kg of Gd-DTPA (Magnevist; Bayer Schering Pharma, Berlin, Germany). If more than one metastatic lesion was found in the brain parenchyma, the patient was asked to return for additional contrast-enhanced MRI at 3.0T with the high-relaxivity agent Gd-BOPTA. Patients were asked to enroll only if they were not to undergo radiation therapy or surgery, and were ready to return for one additional contrast-enhanced MRI study on a sepa-rate day. Eighteen patients (14 men and four women) met the entrance criteria and were enrolled in the study. All had histologically confi rmed lung carcinoma. The mean patient age was 60 years (age range: 46–77 years).
All studies were performed using a clinical 1.5T MRI whole-body imaging unit (Signa Excite HD 1.5 T; GE Healthcare, Milwaukee, Wisc., USA) with a peak gradient strength of 40 mT/m and a 3.0T MRI (Signa Excite HD 3.0 T; GE Healthcare, Milwaukee, Wisc., USA) with a peak gradient strength of 50 mT/m. Birdcage head coils were used with both units. In addition, both units were equipped with actively shielded gradient systems (slew rate 150 mT/m/ms). The fi rst examina-tion at 1.5T and the second one at 3.0T were performed at least 24 hours apart (range: 24 to 46 hours).
At 1.5T, we used a series of standard MR pulse sequences that are routinely used at our hospital, including fast spin-echo (FSE) T2-weighted imaging in the sagittal plane with 3-mm section thickness, fol-lowed by FSE T2-weighted imaging, spin-echo (SE) T1-weighted imaging, and fl uid-attenuated inversion recovery (FLAIR) imaging in the transverse plane. After contrast material administration, SE T1-weighted images were acquired in the transverse, coronal, and sagittal planes. All images in the transverse plane were parallel to the anterior commissure–posterior commis-sure line on the sagittal T2-weighted images. The SE T1-weighted sequence parameters included a repetition time (TR) of 500 ms and an echo time (TE) of 12 ms, a fi eld of view of 230 mm, a 256 X 205 matrix, a section thickness of 5 mm, an intersection gap of 1 mm, and a bandwidth of 31.25 Hz/pixel.
The contrast agent Gd-DTPA was administered intra-venously using a power injector (Spectris MR Injection System; Medrad, Indianola, Pa., USA) at a fl ow rate of 2 ml/s. Image acquisition was started 1 min after the end of contrast injection.
At 3.0T MRI, FSE T2-weighted images were acquired in the sagittal plane and SE T1-weighted images were acquired in the transverse plane, followed by contrast-enhanced SE T1-weighted images in the transverse plane. Parameters that defi ned image geometry (e.g., thickness, number of sections, matrix) were identical to those used for the 1.5T setting. For SE T1-weighted images, the same TR/TE (500/12 ms) and same band-width that were used for the 1.5T system were used for the 3.0T system. The transverse planar images were parallel to the anterior commissure–posterior commissure line on the sagittal T2-weighted images to ensure that the sections in each patient covered the same anatomical structures as closely as possible. Gd-BOPTA was injected manually using a 5-ml injector. Cumulative doses of 0.025 mmol/kg, 0.05 mmol/kg, 0.075 mmol/kg, and 0.1 mmol/kg (0.1 mmol/kg body weight overall) were given at 5-min intervals over a total period of 20 min. SE T1-weighted images in the transverse plane were acquired 1 min after the end of each injection.
Image sets were transferred to the postprocessing unit. Images from the two studies performed in each patient were loaded onto the screen. All images were reviewed independently by two neuroradiologists (H.-J.L., G.-Y.W.) on a digital picture archiving and communication (PACS) workstation (Centricity; GE Healthcare, Milwaukee, Wisc., USA). The Gd-DTPA-enhanced images (1.5T) were reviewed fi rst, followed by Gd-BOPTA-enhanced images (3.0T) at different doses in random order. The readers were blinded to the various Gd-BOPTA doses. Images were viewed with standardized window settings (window level of 1000 HU and window width of 1200 HU). Each postcontrast image obtained using the 3.0T unit was compared with the corresponding enhanced image obtained with the 1.5T unit in terms of lesion detection and confi dence for lesion detection. Confi dence was evaluated on the basis of a three-point scale: 1 = Gd-BOPTA provided worse confi dence in terms of lesion detectability; 2 = Gd-BOPTA provided equal confi dence in terms of lesion detectability; and 3 = Gd-BOPTA provided better confi dence in terms of lesion detectability.
Throughout the study, regions of interest (ROIs) were 15–20 mm2 in area and were manually placed by the same author. ROIs were manually placed to select contrast-enhanced tumor tissue and contralateral normal-appearing white matter. To assess background noise, ROIs of the same size were always placed in the same area of ghosting-free image background. Signal intensity and noise values were used to calculate the SNR. To determine CNR of enhancing lesions, the SNR of the contralateral normal-appearing frontal white matter (SNRWM) was subtracted from the SNR of contrast-enhanced lesions (SNRL) with use of the following equation:
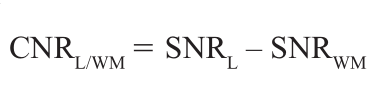
where CNRL/WM is the CNR between enhancing lesions and cerebral white matter. For each of the 18 patients, the CNRL/WM was calculated for the study performed at 3.0T with a specifi c cumulative dose of Gd-BOPTA (0.025 mmol/kg, 0.05 mmol/kg, 0.075 mmol/kg, or 0.1 mmol/kg) and for the study performed at 1.5T with 0.1 mmol/kg Gd-DTPA. The median and average values of the fi ve independent CNR calculations were determined.
The relative CNR (rCNR) was calculated in order to quantify the effect of Gd-BOPTA and higher mag-netic fi eld strength on lesion-to-brain CNR for each patient. The ratio represents each patient’s CNR between enhancing lesions and normal-appearing cere-bral white matter at 3.0T using Gd-BOPTA relative to the same patient’s CNR between enhancing lesions and normal-appearing cerebral white matter at 1.5T using contrast GD-DTPA, according to the following equation:
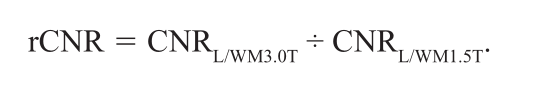
Statistical analysis was performed using SPSS soft-ware (version 10.0.1; SPSS Inc., Chicago, Ill., USA). The Wilcoxon matched-pairs signed-rank test was used to test the distribution of CNR for individual lesions obtained with the 3.0T unit with cumulative doses of 0.025 mmol/kg, 0.05 mmol/kg, 0.075 mmol/kg, and 0.1 mmol/kg of Gd-BOPTA as compared with those obtained with the 1.5T unit with 0.1 ml/kg Gd-DTPA. A P value of <0.05 indicated a statistically signifi cant difference.
Results
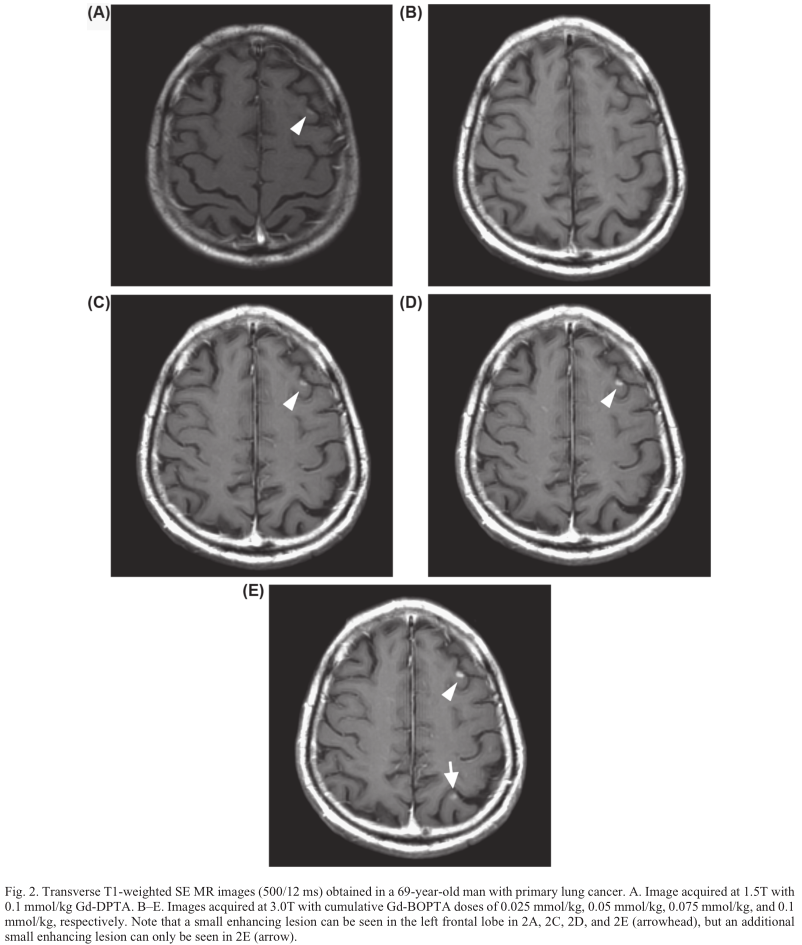
Among the 18 patients, lesion conspicuity was rated highest on images obtained at 3.0T with 0.1 mmol/kg Gd-BOPTA (median score, 3), whereas conspicuity on images obtained at 3.0T with cumulative doses of 0.05 mmol/kg and 0.075 mmol/kg Gd-BOPTA was rated as equivalent to that obtained at 1.5T with Gd-DTPA (median score, 2). Lesion conspicuity was rated lowest on images obtained at 3.0T with 0.025 mmol/kg Gd-BOPTA (median score, 1) (Fig. 1). For images acquired with 0.025 mmol/kg and 0.05 mmol/kg Gd-BOPTA at 3.0T, no increase in number of lesions was identifi ed by the two readers as compared with images enhanced with Gd-DTPA at 1.5T. There was an increase in the number of lesions identifi ed at 3.0T with 0.075 ml/kg Gd-BOPTA compared with images enhanced with Gd-DTPA at 1.5T (Fig. 2) in three patients (17%), as graded by both assessor 1 and 2. In addition, for images acquired with a 0.1-ml/kg dose of Gd-BOPTA at 3.0T, there was an increase in the number of lesions identi-fi ed compared with images enhanced with Gd-DTPA at 1.5T in four patients (22%) as graded by assessor 1, and three patients (17%) as graded by assessor 2.
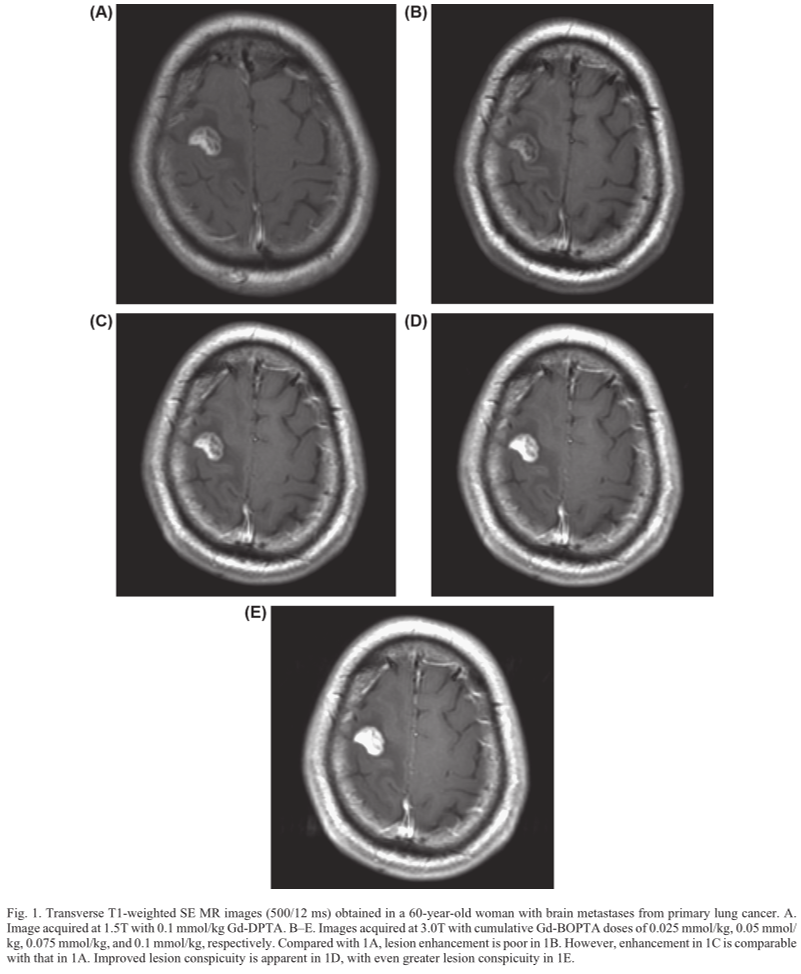
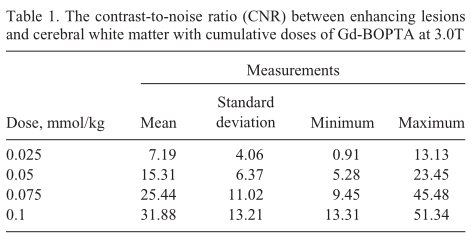
For imaging at 1.5T with standard 0.1 ml/kg Gd-DTPA, the median CNR between enhancing lesions and normal-appearing contralateral cerebral white matter was 12.17, with a mean of 12.01 ± 2.53. In comparison, for the 3.0T imaging with cumulative Gd-BOPTA doses of 0.025 mmol/kg, 0.05 mmol/kg, 0.075 mmol/kg, and 0.10 mmol/kg, the median CNR was 8.2, 17.0, 36.0, and 38.0, respectively. The corresponding mean values were 7.19 ± 4.06, 15.31 ± 6.37, 25.44 ± 11.02, and 31.88 ± 13.21, respectively (Table 1).
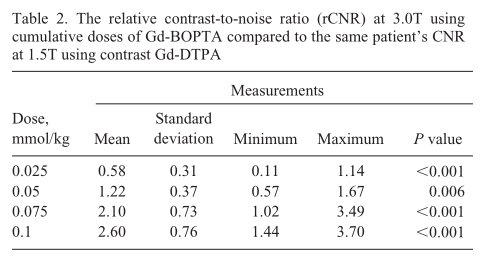
The 3.0T imaging with 0.025 mmol/kg Gd-BOPTA showed a decrease in CNR between enhancing lesions and contralateral normal-appearing cerebral white matter compared with 1.5T studies using 0.1 mmol/kg Gd-DTPA. The median rCNR was 0.60, with a mean of 0.58 ± 0.31 (P < 0.001, Wilcoxon signed-rank test). However, changes in CNR increased with cumulative Gd-BOPTA doses of 0.05 mmol/kg, 0.075 mmol/kg, and 0.10 mmol/kg. The corresponding median rCNRs were 1.34, 2.13, and 2.73, respectively, and the corresponding means were 1.22 ± 0.37 (P <0.01), 2.10 ± 0.73 (P <0.001), and 2.60 ± 0.76 (P <0.001), respectively (Table 2).
Discussion
Metastases are among the most common brain neoplasms, accounting for nearly 37% of all adult brain tumors (11). This rapidly growing incidence is likely due to the growing effectiveness of therapies for primary malignant tumors and improved detection with new CNS imaging modalities (12). The standard dose of contrast is 0.1 mmol/kg for detection of brain metastases on a 1.5T MR imaging system (1). Our study demonstrated that a lower dose (0.05 mmol/kg) of Gd-BOPTA at 3.0T can achieve higher CNR for patients with brain metastases compared to an exami-nation using 0.1 mmol/kg Gd-DTPA at 1.5T, with a median rCNR of 1.34 (P < 0.01). A lower dose of con-trast material can also be considered benefi cial in terms of patient acceptability, because a lower injection dose is likely to result in fewer side effects compared to a higher dose.
Currently, several gadolinium-based MRI con-trast agents are used to image the CNS, and there are several differences among these agents. Agents For Gd-DPTA, the R1 relaxivity was 3.9 l·mmol-1·s-1 for both 1.5T and 3.0T. The high R1 relaxivity for Gd-BOPTA may be expected to lower the overall dose nec-essary for scanning compared with the 0.1-mmol/kg dose commonly used with Gd-DTPA.
One of the main features of MRI at 3.0T is the general gain in SNR compared with that at lower fi eld strengths. Accordingly, signal intensity changes caused by con-trast enhancement observable on T1-weighted images should generally be stronger at 3.0T than they are at 1.5T (6, 7). In our study, a dose of 0.05 mmol/kg Gd-BOPTA not only signifi cantly improved the sensitivity for lesion detection compared to unenhanced 3.0T MRI, but also can be considered equivalent to 0.01 mmol/kg Gd-DTPA at 1.5T in terms of contrast enhancement and diagnostic effi cacy. However, a dose of 0.1 mmol/kg of Gd-BOPTA at 3.0T could provide even greater improve-ment in lesion detection, delineation, and conspicuity.
considered “fi rst generation” include Magnevist (Gd-DTPA; Bayer), ProHance (Gd-HP-DO3A, gadot-eridol; Bracco), Omniscan (Gd-DTPA-BMA, gadodi-amide; GE Healthcare), Optimark (Gd-DTPA-BMEA, gadover setamide; Tyco), Dotarem (Gd-DOTA, gadot-erate meglumine; Guerbet), and Gadovist (Gd-DO3A-butrol, gadobutrol; Bayer). These agents have similar T1 relaxivity values, ranging between 4.3 and 5.6 l·mmol-1·s-1 for 1.5T MRI systems (13). The “second-generation” gadolinium-based compound Gd-BOPTA has become commercially available for CNS imaging in recent years. Because of weak, transient protein binding, Gd-BOPTA possesses enhanced R1 and R2 relaxivities and, therefore, faster transverse and longitudinal relaxation and recovery rates compared with the other gadolini-um-based MRI contrast agents. These faster transverse and longitudinal relaxation and recovery rates result in signifi cantly increased contrast enhancement. BLEICHER et al. (14) demonstrated higher R1 and R2 relaxivities of Gd-BOPTA relative to other commercially available gadolinium contrast agents using a contrast phantom with serial dilutions of different contrast agents. These differences are present using both 1.5T and 3.0T units. ROHRER et al. (15) found that R1 relaxivities for Gd-BOPTA were 6.3 l·mmol-1·s-1 at 1.5T and 5.5 l·mmol-1·s-1 at 3.0T in plasma at 37°C. For Gd-DPTA, the R1 relax-ivities were 4.1 l·mmol-1·s-1 at 1.5T and 3.7 l·mmol-1·s-1 at 3.0T. However, according to PINTASKE et al. (16), the R1 relaxivity of Gd-BOPTA was 7.9 l·mmol-1·s-1 at 1.5T and 5.9 l·mmol-1·s-1 at 3.0T in human blood plasma (37°C).
With 1.5T MR imaging as a reference standard, KRAUTMACHER et al. (17) investigated the effect of different doses of Gd-DTPA on CNR at 3.0T in patients with primary and secondary brain tumors, and showed that CNR increased more than twofold at 3.0T compared with 1.5T imaging, with a median relative CNR of 2.8. Moreover, even with half the dose of contrast agent, the CNR at 3.0T was signifi -cantly higher (ratio of change in CNR with half dose, median, 1.3 fold) compared with the same patient’s examination at 1.5T. The changes in CNR between 1.5T and 3.0T were similar to those found by KRAUT-MACHER et al., although KRAUTMACHER’s group used Gd-DTPA at both fi eld strengths. Compared with their study, no better CNR improvements were observed in our study. This may be explained by the fact that our study lesions were comprised only of brain metastases, whereas the patients in KRAUT-MACHER’s group consisted of both primary and sec-ondary brain tumors. It was confi rmed in a rat glioma study that Gd-BOPTA is superior to Gd-DTPA in neurologic imaging at 3.0T, and that Gd-BOPTA can provide signifi cantly higher CNR at 3.0T compared with 1.5T (18). Recently, a study was conducted to confi rm that qualitative and quantitative depiction of brain lesions at 3.0T was signifi cantly improved using 0.1 mmol/kg Gd-BOPTA compared to brain imaging with Gd-DTPA at equivalent doses (19).
It was also demonstrated that studies performed at 1.5T with a cumulative contrast dose of 0.3 mmol/kg gadot-eridol allowed detection of additional brain metastases in approximately 20% of patients. Although they detected highly signifi cant differences in small lesions, there was no difference in detection rate for lesions larger than 10 mm (20, 21). Our data showed that using 0.05 mmol/kg Gd-BOPTA at 3.0T produced results similar to those obtained using 0.1 mmol/kg Gd-DTPA at 1.5T. We did note that cumulative doses of 0.075 mmol/kg and 0.1 mmol/kg improved lesion detection, but the lesions were always small with a diameter of less than 5 mm.
One of the limitations of this study is that our lesions were comprised only of brain metastases, so we cannot know whether a low dose (0.05 mmol/kg) of Gd-BOPTA can achieve the same diagnostic effi cacy for other types of brain tumors at 3.0T. Further inves-tigation with a larger group of patients with different primary tumors is necessary to answer this question. In addition, the number of patients in our study was small, making the sensitivity data less robust than the specifi city data. In the present study, the patients were fi rst screened at 1.5T, so the readers might have known which images were scanned at 1.5T using Gd-DTPA. The 1-min imaging delay after contrast administra-tion that we used may be too short a time and may also represent a limitation of our study.
In conclusion, our data suggest that assessment of possible brain metastases using 0.05 mmol/kg Gd-BOPTA with a 3.0T MR imaging system is com-parable to 0.1 mmol/kg Gd-DTPA at 1.5T. However, a dose of 0.1 mmol/kg at 3.0T improved lesion detec-tion delineation and conspicuity, as compared to 0.1 mmol/kg Gd-DTPA at 1.5T, leading to greater confi -dence among our radiologists in their ability to detect or exclude metastatic lesions.
Declaration of interest: The authors report no confl icts of interest. The authors alone are responsible for the content and writing of the paper.
References
1. Schellinger PD, Meinck HM, Thron A. Diagnostic accuracy of MRI compared to CCT in patients with brain metastases. J Neurooncol 1999;44:275–81.
2. Akeson P, Larsson EM, Kristoffersen DT, Jonsson E, Holtas S. Brain metastases—comparison of gadodi- amide injection-enhanced MR imaging at standard and high dose, contrast-enhanced CT and non-contrast-enhanced MR imaging. Acta Radiol 1995;36:300–6.
3. Haustein J, Laniado M, Niendorf HP, Louton T, Beck W, Planitzer J, et al. Triple-dose versus standard-dose gado- pentetate dimeglumine: a randomized study in 199 patients. Radiology 1993;186:855–60.
4 .Sze G, Johnson C, Kawamura Y, Goldberg SN, Lange R, Friedland RJ, et al. Comparison of single- and triple-dose contrast material in the MR screening of brain metastases. Am J Neuroradiol 1998;19:821–8.
5. Runge VM, Wells JW, Nelson KL, Linville PM. MR imaging detection of cerebral metastases with a single injection of high- dose gadoteridol. J Magn Reson Imaging 1994;4:669–73.
6. Wintersperger BJ, Runge VM, Biswas J, Reiser MF, Schoenberg SO. Brain tumor enhancement in MR imaging at 3 Tesla: comparison of SNR and CNR gain using TSE and GRE techniques. Invest Radiol 2007;42:558–63.
7. Biswas J, Nelson CB, Runge VM, Wintersperger BJ, Baumann SS, Jackson CB, et al. Brain tumor enhancement in magnetic resonance imaging: comparison of signal-to- noise ratio (SNR) and contrast-to-noise ratio (CNR) at 1.5 versus 3 Tesla. Invest Radiol 2005;40:792–7.
8. Knopp MV, Runge VM, Essig M, Hartman M, Jansen O, Kirchin MA, et al. Primary and secondary brain tumors at MR imaging: bicentric intraindividual crossover compar- ison of gadobenate dimeglumine and gadopentetate dime- glumine. Radiology 2004;230:55–64.
9. Kirchin MA, Pirovano GP, Spinazzi A. Gadobenate dimeglumine (Gd-BOPTA). An overview. Invest Radiol 1998;33:798–809.
10. Baleriaux D, Colosimo C, Ruscalleda J, Korves M, Schneider G, Bohndorf K, et al. Magnetic resonance imaging of metastatic disease to the brain with gadobenate dimeglumine. Neuroradiology 2002;44:191–203.
11. Vecht CJ. Clinical management of brain metastasis. J Neurol 1998;245:127–31.
12. Takeda T, Takeda A, Nagaoka T, Kunieda E, Takemasa K, Watanabe M, et al. Gadolinium-enhanced three-dimen- sional magnetization-prepared rapid gradient-echo (3D MP-RAGE) imaging is superior to spin-echo imaging in delineating brain metastases. Acta Radiol 2008;49: 1167–73.
13. Essig M. MR imaging of CNS tumors: are all contrast agents created the same? Neuroradiology 2006;48 Suppl 1:3–8.
14. Bleicher AG, Kanal E. A serial dilution study of gado- linium-based MR imaging contrast agents. Am J Neurora- diol 2008;29:668–73.
15. Rohrer M, Bauer H, Mintorovitch J, Requardt M, Weinmann HJ. Comparison of magnetic properties of MRI contrast media solutions at different magnetic fi eld strengths. Invest Radiol 2005;40:715–24.
16. Pintaske J, Martirosian P, Graf H, Erb G, Lodemann KP, Claussen CD, et al. Relaxivity of gadopentetate dimeglu- mine (Magnevist), gadobutrol (Gadovist), and gadobenate dimeglumine (MultiHance) in human blood plasma at 0.2,1.5, and 3 Tesla. Invest Radiol 2006;41:213–21. Erratum in Invest Radiol 2006;41:859.
17. Krautmacher C, Willinek WA, Tschampa HJ, Born M, Traber F, Gieseke J, et al. Brain tumors: full- and half-dose contrast-enhanced MR imaging at 3.0 T compared with 1.5T—initial experience. Radiology 2005;237:1014–9.
18. Runge VM, Biswas J, Wintersperger BJ, Baumann SS, Jackson CB, Herborn CU, et al. The effi cacy of gadobenate dimeglumine (Gd-BOPTA) at 3 Tesla in brain magnetic resonance imaging: comparison to 1.5 Tesla and a standard gadolinium chelate using a rat brain tumor model. Invest Radiol 2006;41:244–8.
19. Rumboldt Z, Rowley HA, Steinberg F, Maldjian JA, Ruscalleda J, Gustafsson L, et al. Multicenter, double- blind, randomized, intra-individual crossover comparison of gadobenate dimeglumine and gadopentetate dimeglumine in MRI of brain tumors at 3 Tesla. J Magn Reson Imaging 2009;29:760–7.
20. Yuh WT, Tali ET, Nguyen HD, Simonson TM, Mayr NA, Fisher DJ. The effect of contrast dose, imaging time, and lesion size in the MR detection of intracerebral metastasis. Am J Neuroradiol 1995;16:373–80.
21. Brekenfeld C, Foert E, Hundt W, Kenn W, Lodeann KP, Gehl HB. Enhancement of cerebral diseases: how much contrast agent is enough? Comparison of 0.1, 0.2, and 0.3 mmol/kg gadoteridol at 0.2 T with 0.1 mmol/kg gadot- eridol at 1.5 T. Invest Radiol 2001;36:266–75.