1 , Biao Huang a , 1 , Shuixing Zhang a , 1 , Zaiyi Liu a , ∗ , Changhong Liang a , 1 , b , Chunling Liu a
ABSTRACT
Objectives: To obtain perfusion as well as diffusion information in normal breast tissues and breast lesions from intravoxel incoherent motion (IVIM) imaging with biexponential analysis of multiple b-value diffusion-weighted imaging (DWI) and compare these parameters to apparent diffusion coefficient (ADC) obtained with monoexponential analysis in their ability to discriminate benign lesions and malignant tumors.
Materials and methods: In this prospective study, informed consent was acquired from all patients. Eighty- four patients with 40 malignant tumors, 41 benign lesions, 30 simple cysts and 39 normal breast tissues were imaged at 1.5 T utilizing contrast-enhanced magnetic resonance imaging (MRI) and DWI using 12 b values (range: 0–1000 s/mm 2 ). Tissue diffusivity (D), perfusion fraction (f) and pseudo-diffusion coef- ficient (D*) were calculated using segmented biexponential analysis. ADC (b = 0 and 1000 s/mm 2 ) was calculated with monoexponential fitting of the DWI data. D, f, D* and ADC values were obtained for nor- mal breast tissues, simple cysts, benign lesions and malignant tumors. Receiver operating characteristic analysis was performed for all DWI parameters.
Results: There was good interobserver agreement on the measurements between the 2 observers. D values were significantly different among malignant tumors, benign lesions, simple cysts and normal breast tissues (P = 0.000) and it was the same result for f, D* and ADC values. Further comparisons of these 4 parameters between every single pair were as the following. D and ADC values of malignant tumors were significantly smaller than those of benign lesions, simple cysts and normal tissues (P = 0.000, respectively).
The f value of malignant tumors was significantly higher than that of benign lesions, simple cysts and normal breast tissues (P = 0.001, P = 0.000, and P = 0.000). D and ADC values demonstrated higher sensitivity and specificity in differentiating benign lesions and malignant tumors, with area under the curve (AUC) of 0.952 and 0.945, respectively, while f and D* with the lower AUC of 0.723 and 0.630, respectively. Combining f and D values had a sensitivity up to 98.75%. Conclusion: DWI response curves in malignant tumors, benign lesions and normal fibroglandular tissues are found to be biexponential fit in comparison with the monoexponential fit for simple cysts. IVIM provides separate quantitative measurement of D for cellularity and f and D* for vascularity and is helpful for differentiation between benign and malignant breast lesions。
1. Introduction
It is well known that conventional mammography is the basic method used for screening breast cancer, but it has only a sensibility of 69–90% [1,2] and the sensibility may be decreased by 48% in cases of dense breast parenchyma [1]. Dynamic contrast-enhanced MRI of the breast has recently been demonstrated to be the most sensitive breast screening technique for women at high risk and the sensitivity in the differentiation of the malignant lesions from the benign ones is 90–95%, while a wide variation in the specificity and positive predictive value has been found to be from 46% to 97% [3]. According to a published meta-analysis, contrast-enhanced breast MRI provides an overall sensitivity of 90% and specificity of 72% in exploring breast lesions [4]. Thus, the differentiation of a benign or malignant lesion detected on MRI still remains a challenge [5].
Diffusion-weighted imaging (DWI) is a non contrast-enhanced type of MRI which is most simply performed with 2 b values, such as 0 and 1000 s/mm 2 . The exponential decay of signals is proposed based on the assumption of the monoexponential fit to arrive at a decay constant, referred to as the apparent diffusion coefficient (ADC) value. Many studies have demonstrated the usefulness of ADC value of DWI in the differential diagnosis of breast lesions [6–14]. The reported sensitivity and specificity classified as malig-nant tumors by DWI ranged from 62.5% to 92.8% and 45.8% to 96.7%, respectively. In a recent meta-analysis of quantitative DWI in the differential diagnosis of breast lesions, the overall sensitivity and specificity in one homogenous subgroup of studies using maximum b = 1000 s/mm2 were 0.84 and 0.84 respectively [15]. DWI has a higher specificity compared to that of contrast-enhanced MRI, how-ever, in the meta-analysis, different maximum b values were used, including 400, 500, 600, 750, 800, 1000 and 2000 s/mm2, which resulted in the different threshold from 0.90 to 1.60 × 10−3 mm2/s. Even with the same maximum b value, the thresholds still were different. Therefore, results from DWI must be explained with cau-tion.
In vivo, microscopic motion of water molecules detected by DWI is influenced not only by diffusion of water molecules, affected by the structures of the tissue, but also by microcirculation of blood in the capillary network [16]. Accordingly, the signal attenuation on monoexponential DWI sometimes does not represent a linear relationship and it is difficult to calculate the accurate ADC value. Intravoxel incoherent motion (IVIM), first described by Le Bihan et al. [17], is an interesting imaging technique for the separate esti-mation of tissue perfusion and diffusivity using multi-b-value DWI, followed by biexponential curve fit. Such analysis from IVIM can resolve pure diffusion coefficient (D) and perfusion-related inco-herent microcirculation (D*) separately, along with microvascular volume fraction (f). In recent years, with the improved MR hard-ware, a renewed interest in IVIM has been shown on prostate [16], liver [18], salivary gland [19], kidney [20] and so on, and the appli-cations of IVIM on breast lesions have been reported, but relatively rarely [21].
The purpose of this study is to prospectively compare the IVIM parametric maps (D – tissue diffusivity, f – perfusion fraction and D* – pseudo-diffusion coefficient) obtained with multi-b values on normal breast tissue, benign lesions and malignant tumors and to determine whether these parameters can distinguish benign from malignant breast lesions with higher accuracy, comparing with ADC monoexponential fit.
2. Materials and methods
2.1. Patients
The project of this prospective study was agreed by the ethics committee of our hospital, and informed consent was acquired from all patients. From July 2012 to February 2013, DWI exami-nations were performed in 84 patients (mean age, 48 years, range, 20–76 years; all of them are females) with a total of 111 breast lesions. Benign lesions included 30 patients with 41 lesions (mean size, 17.45 ± 1.51 mm) and 20 patients with 30 simple cysts (mean size, 21.23 ± 2.90 mm). The malignant tumors included 34 patients with 40 lesions (mean size, 17.70 ± 3.04 mm). The 41 benign lesions consisted of 30 fibroadenomas, 9 lesions with hyperplasia and adenosis of breast, 1 intraductal papillomas and 1 breast abscess. The 40 malignant tumors consisted of 29 invasive ductal carcinoma (IDC), 1 glycogen-rich clear cell carcinoma, 4 ductal carcinoma in situ (DCIS), 2 infiltrating lobular carcinoma, 4 nonspecific inva-sive breast carcinoma. The final diagnosis was established on the basis of histopathology of surgical excised specimens in 65 lesions (24 malignant tumors, 30 benign lesions and 11 cysts), needle biopsy specimens in 20 lesions (16 malignant tumors and 4 benign lesions), stable lesions during over 3-year follow up in 7 benign lesions and breast contrast-enhanced dynamic MRI and ultrasound in the residuary 19 cysts. In addition, we evaluated the IVIM parameters and ADC values of healthy breast tissues on the 39 contralateral sides.
2.2. Conventional MR Imaging
MR imaging was performed by using a 1.5-T MR imager (Achieva 1.5 T, Philips Healthcare, Best, Netherlands) equipped with a 4-channel SENSE breast coil in prone position. Axial T1-weighted (repetition time (TR)/echo time (TE), 4.8/2.1 ms; field of view (FOV), 300 × 320 mm2) and T2-weighted fat-suppressed (spectral presat-uration attenuated inversion recovery, SPAIR) (TR/TE, 3400/90 ms; FOV 320 × 260 mm2; reconstruction matrix, 348 × 299; slice thick-ness/gap, 3/0.3 mm) images of breast were obtained.
2.3. Contrast-enhanced MRI
A gadolinium-based agent Gd-DTPA (gadopentetate dimeg-lumine, Magnevist; Bayer Healthcare, Berlin, Germany) was intravenously injected at a dose of 0.2 ml/kg of body weight and at a rate of 1.5 ml/s, followed by a 20-ml saline flush with high pressure injector. Axial 3D T1-weighted fat-saturated images were obtained just before contrast and at 9 consecutive time points (duration 30 s each) following the administration of Gd-DTPA contrast agent.
2.4. DW MR imaging
Axial DW images were obtained by using single-shot spin-echo echo-planar imaging (EPI) before administration of Gd-DTPA. Axial DWI images with bilateral breast coverage were collected (TR/TE, 5065/66 ms; FOV, 300 × 300 mm2; acquisition matrix 200 × 196; slice thickness/gap, 5/1 mm) with spectral presaturation inversion recovery (SPIR) and diffusion sensitization in the anterior-posterior direction applied with weighting factors of b 0, 10, 20, 30, 50, 70, 100, 150, 200, 400, 600 and 1000 s/mm2. Total scan time for the IVIM scan was 227 s.
2.5. Image analysis
The bi-exponential model from an IVIM sequence was expressed by the following equation, as described by Le Bihan et al. [22]:
![]()
where Sb is the signal intensity in the pixel with diffusion gradient b, S0 is the signal intensity in the pixel without diffusion gradient, D is the true diffusion as reflected by pure molecular diffusion, f is the fractional perfusion related to microcirculation, and D* is the pseu-dodiffusion coefficient representing perfusion-related diffusion or incoherent microcirculation.
All image analysis were performed with a manufacturer-supplied software (PRIDE DWI Tool, version 1.5, Philips Healthcare) and fitted on a pixel-by-pixel basis using the Levenberg–Marquardt algorithm, as described before [23]. The three parameters were calculated consecutively in which D was obtained by a simplified linear fit equation (Sb = S0 × exp−bD) using b values > 200 s/mm2. This was based on the assumption that D* is significantly greater than D such that its influence on signal decay can be neglected for b values > 200 s/mm2. f and D* were calculated by using a non-linear regression algorithm for all b values.
For the current data analysis, the PRIDE software will calculate the goodness of fit, R2, pixel by pixel. The goodness of fit of data collected in this current study was above 0.8. If the fit of data was less than 0.8, then the data were excluded from this study.
2.6. Image post-processing and regions of interest (ROI)
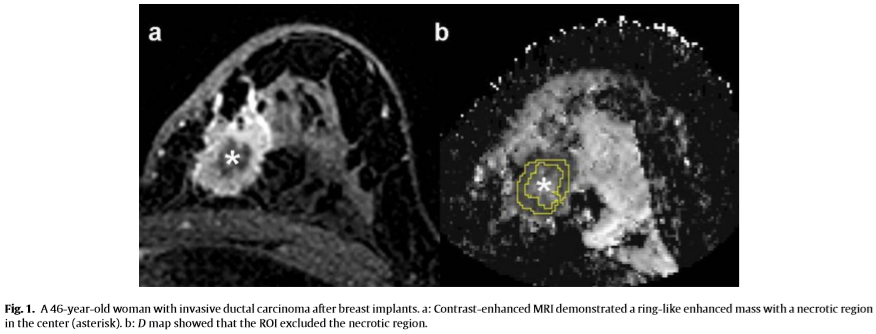
Diffusion-weighted imaging data were transferred to a computer equipped with a manufacturer-supplied software (PRIDE DWI Tool, version 1.5, Philips Healthcare) and work-station (Extended Workspace, Philips Healthcare), for IVIM and mono-exponential analysis, respectively. ROI measurements of IVIM parametric maps were obtained with Image J software (National institute of Health, Bethesda, MD). Conventional and contrast-enhanced T1-weighted MR images and DWI images (b = 1000 s/mm 2 ) were used as references to determine lesion areas on the corresponding ADC maps and IVIM parametric maps. ROI was manually placed on each lesion at the level of maximum trans- verse diameter of lesions and were chosen to be as large as possible, consistent with minimal contaminations from surrounding unin- tended tissues. Large cystic or necrotic areas by visual inspection (Fig. 1) were excluded from ROI in order to focus upon viable tumor tissue in deriving IVIM parameters and ADC values. The mean ROI area was 98 mm 2 (range, 15–392 mm 2 ). For the IVIM parameters measurements, firstly, a ROI was drawn on D map because of the good SNR, and then it was copied to the f and D* map with Image J software and the ROI on D map might be adjusted according to f and D* map. For a mono-exponential analysis, ADC values were measured on ADC maps produced from b = 0 and 1000 s/mm 2 and the ROIs were kept as close as possible to those on IVIM parametric maps. For the contralateral healthy breast fibroglandular tissues, the sizes of ROIs were in a range of 100–200 mm 2 and excluded large vessels and ducts. D, f, D* and ADC values were measured by 2 independent observers (with experiences of 7 and 20 years of breast MRI diagnosis).
2.7. Statistical analysis
SPSS Statistics V17.0 was used for the statistics analysis. The intraclass correlation coefficient (ICC) was calculated to derive the data variability for the 2 different observers. All the lesions and normal breast tissues were compared in terms of each DWI parameters (D, f, D* and ADC) using mixed model analysis of variance. Test of normal distribution for each group and each IVIM parameter and ADC value was performed. The parameters were compared in different groups by K independent samples test, respectively and Mann–Whitney U test was used for further comparisons between specific group pairs (Malignant vs. Benign, Malignant vs. Cyst, Malignant vs. Normal, Benign vs. Cyst, Benign vs. Normal, Cyst vs. Normal) (P < 0.008 was thought to be statistically significant because of 6 times of comparisons between groups). Receiver operating characteristic (ROC) curve analyses were per- formed to assess the utility of the measures for the detection of benign and malignant lesions and to identify thresholds to be used in a test to detect malignant tumors. Parallel test (Sensitiv- ity A + (1 − Sensitivity A) × Sensitivity B) was used to calculate the sensitivity of combining D and f values. Comparison of ROC curves for IVIM parameters and ADC value was done by Medcalc (MedCalc Software, Acacialaan 22, B-8400 Ostend, Belgium). D values were compared with ADC values for different groups by paired-samples t test.
3. Results
3.1. Signal decay curves of normal and pathologic breast tissues
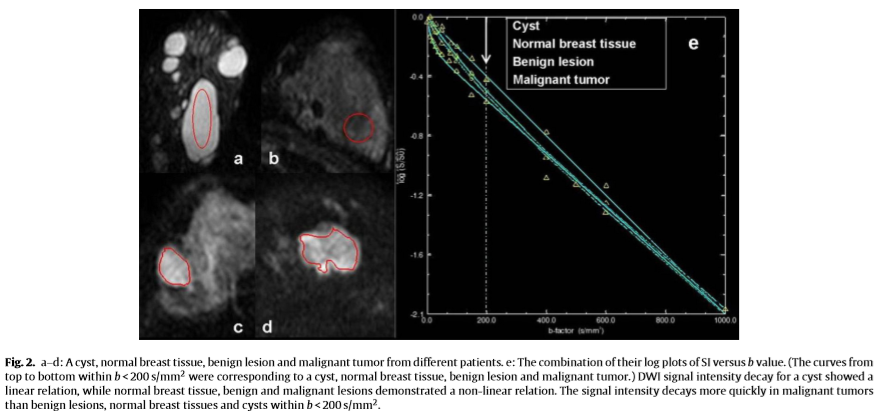
The relative signals of the normal and pathologic breast tis- sue decayed with a large-range b values (Fig. 2). However, normal breast tissue, cysts, benign lesions and malignant tumors had their distinctive signal decay curve profiles, which implied that they had unique IVIM parameters.
3.2. Interobserver agreement
There was excellent interobserver agreement between the 2 observers in measure of monoexponential fit parameter ADC value with ICC of 0.995 (95% CI: 0.993–0.996). Similarly, there were excellent interobserver agreements in IVIM parameters D, with ICC of 0.997 (95% CI: 0.996–0.998) and f with ICC of 0.962 (95% CI: 0.948–0.972), and a relatively good ICC for D* with ICC of 0.883 (95% CI: 0.842–0.914). The result suggested excellent agreement between the 2 readers for all DWI measures.
3.3. Biexponential and monoexponential fitting DWI results
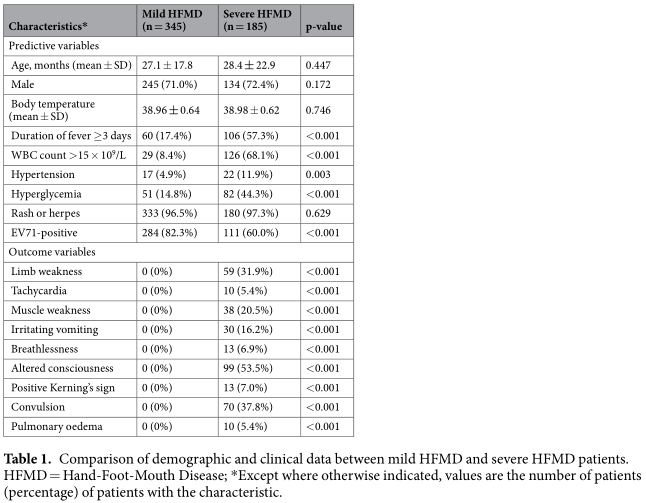
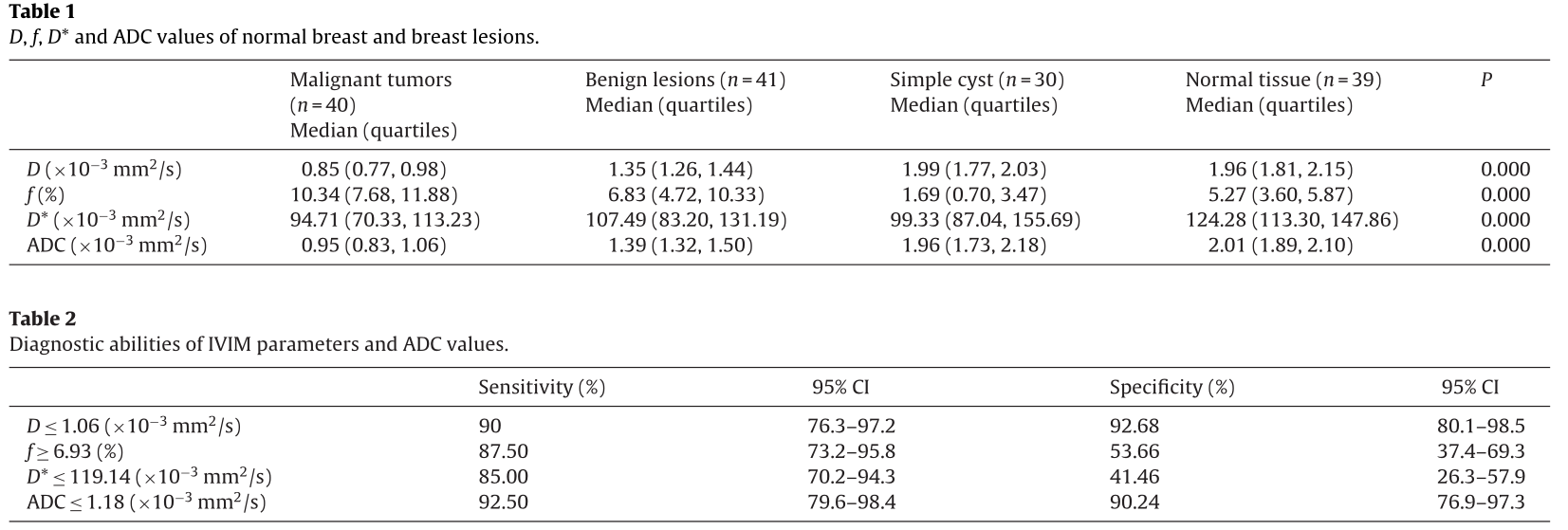
D, f and D* values from IVIM biexponetial fitting and ADC value from monoexponential fitting (b = 0, 1000 s/mm 2 ) of the normal breast tissues and breast lesions were shown in Table 1. The Kruskal–Wallis test demonstrated significant differences in IVIM parameters and ADC values among malignant tumors, benign lesions, simple cysts and normal breast tissues (X2 = 122.565, P = 0.000 for D, X 2 = 87.585, P = 0.000 for f,X 2 = 16.000, P = 0.000 for D*, X 2 = 120.122, P = 0.000 for ADC).
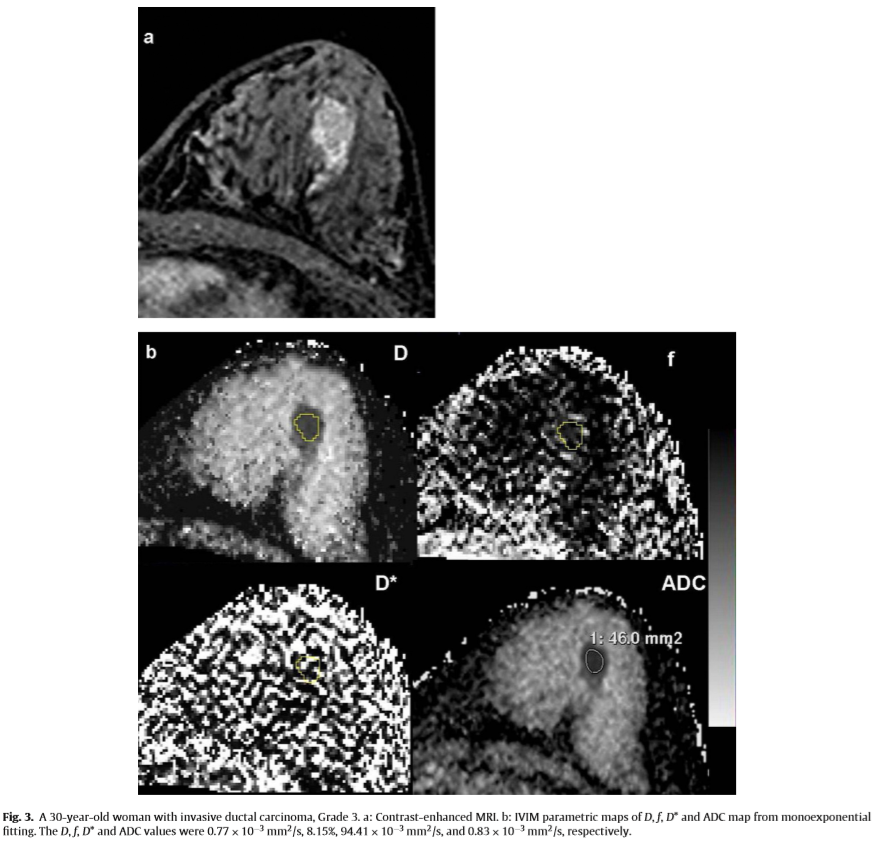
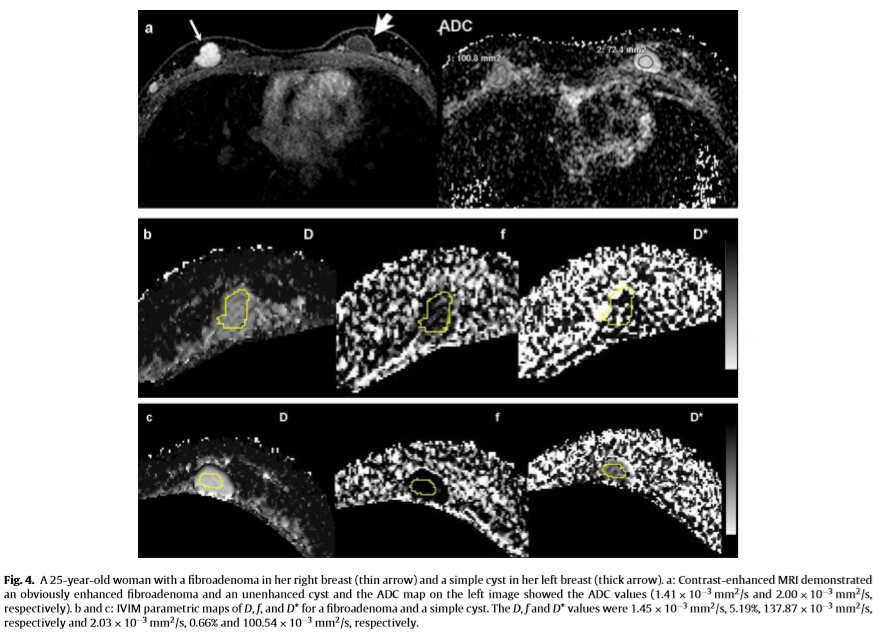
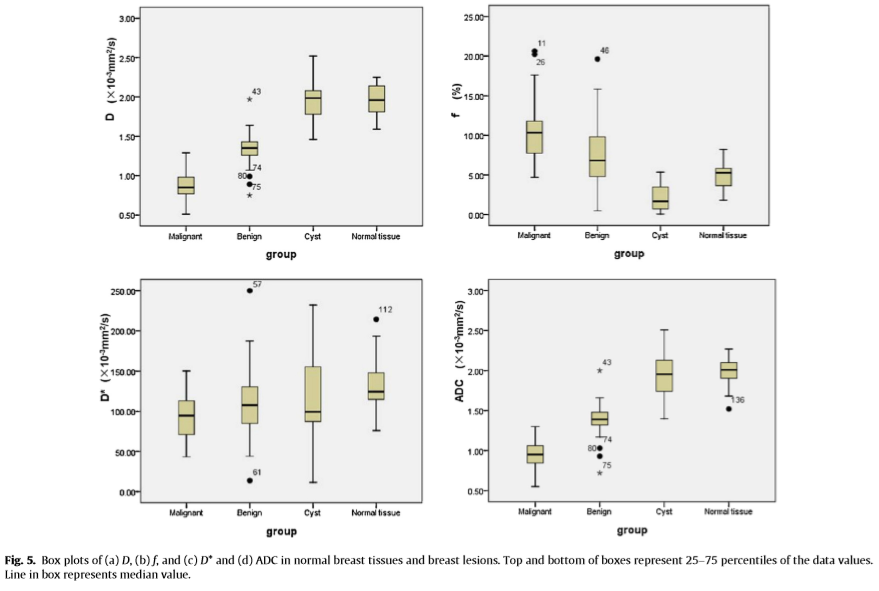
D values of malignant tumors (Fig. 3b) were significantly smaller than those of benign lesions (Fig. 4b), simple cysts (Fig. 4c) and normal tissues (Z = −7.006, P = 0.000; Z = −7.122, P = 0.000 and Z = −7.649, P = 0.000, respectively). D values were also statisti- cally different between benign lesions and cysts or normal tissues (Z = −6.875, P = 0.000 and Z = −7.466, P = 0.000, respectively), while there was no statistical difference of D values between cysts and normal tissues (Z = −0.097, P = 0.923) (Fig. 5a). Using a D value cutoff of 1.06 × 10 −3 mm 2 /s, malignant tumors could be diagnosed with 90% sensitivity and 92.68% specificity (Table 2). The f values of malignant tumors (Fig. 3b) were significantly larger than that of benign lesions (Fig. 4b), simple cysts (Fig. 4c) and normal tissues (Z = −3.457, P = 0.001, Z = −7.097, P = 0.000, and Z = −6.756, P = 0.000, respectively), and it was also statistically dif- ferent between benign lesions and cysts or normal tissues and between cysts and normal tissues (Z = −6.041, P = 0.000, Z = −3.071, P = 0.002 and Z = −5.720, P = 0.000, respectively) (Fig. 5b). Using a cutoff of 6.93%, malignant tumors could be diagnosed with 87.5% sensitivity and 53.66% specificity (Table 2).
D* values of malignant tumors (Fig. 3b) were significantly smaller than that of normal tissues (Z = −4.746, P = 0.000). How- ever, there were no differences between any of the other groups (P < 0.008 was thought to be statistically significant and have been stated that in Section 2.7) (P = 0.043 for malignant and benign lesions (Fig. 4b), P = 0.100 for malignant tumors and simple cysts (Fig. 4c), P = 0.986 for benign lesions and simple cysts, P = 0.013 for benign lesions and normal tissues, and P = 0.019 for cysts and nor- mal tissues) (Fig. 5c). The sensitivity and specificity for diagnosing malignant tumors were very low (Table 2).
Similar trends were noted with ADC value calculated from monoexponential fitting (Fig. 5d). ADC values of malignant tumors (Fig. 3b, ADC) were significantly smaller than those of benign lesions (Fig. 4b), simple cysts (Fig. 4c) and normal tissues (Z = −6.893, P = 0.000, Z = −7.123, P = 0.000, and Z = −7.650, P = 0.000, respectively). ADC values were also statistically different between benign lesions and cysts or normal tissues (Z = −6.450, P = 0.000 and Z = −7.437, P = 0.000), while there was no difference of ADC values between cysts and normal tissues (Z = −0.921, P = 0.357). Using an ADC value cutoff ≤1.18 × 10 −3 mm 2 /s, malignant tumors could be diagnosed with 92.5% sensitivity and 90.24% specificity.
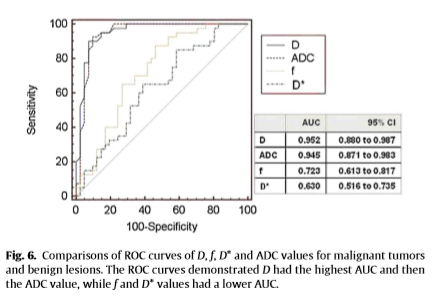
For the comparison between D and ADC values, D values were smaller than ADC values in malignant tumors (t = −8.481, P = 0.000), benign lesions (t = −8.481, P = 0.000) and normal breast tissues (t = −2.148, P = 0.038), but they were almost the same as ADC values in simple cysts (t = 1.410, P = 0.1174). The comparisons of ROC curves of D, f, D* and ADC values (Fig. 6) for discriminating malignant tumors from benign lesions demonstrated D and ADC values had the similar diagnostic efficacy (AUC = 0.952 and 0.945,respectively, Z = 0.9730, P = 0.3306), while f and D* values had a lower diagnostic value (AUC = 0.723 and 0.630). Combining f value, the sensitivity of D value was up to 98.75%.
![]()
4. Discussion
High ADC and D values were found in normal breast tissues and cysts, however inversely, they showed a low f value. The present study turned out there was no difference between D and ADC values in cysts, which implied the micro-perfusion effect did not make contributions to ADC value in cysts. A cyst was almost full of fluid without capillaries, so it was easy to understand the very low f value (f = 1.66%). We had the knowledge that breast was not a highly vascular organ, as demonstrated by the lower blood volume fraction of 1.9% found in normal breast [24] and normal parenchymal enhancement patterns or background enhancement also showed the minimal enhancement and low signal enhance- ment ratio, which indirectly suggested a very low micro-perfusion in normal breast tissues [25,26]. In current study, a non-linear relationship was found between the log(I/I 0 ) and the 12 b values between 0 and 1000 s/mm 2 in normal fibroglandular tissue with a low f value (5.27%). Therefore, the diffusion of normal fibroglandu- lar breast tissue was found to be biexponential. In other words, the biexponential model showed a non-negligibly small perfusion frac- tion, which was consistent with the minimal enhancement. So, the present study did not agree with what Tamura et al. [27] and Baron et al. [28] found, who thought the perfusion effect does not exist in fibroglandular breast tissue. Cysts could be best fitted by a mono- exponential function and IVIM parameters also could reflect the intrinsic characteristics (f values were very low and D values were almost the same as ADC values). The normal fibroglandular tissues could be fitted by a biexponential function and IVIM parameters could show the minute perfusion effect.
We found that D values of malignant tumors were significantly smaller than those of benign lesions, cysts and normal breast tis-sues. The paired-samples T test of D and ADC values between malignant tumors and between benign lesions demonstrated a sig-nificant difference, which implied the micro-perfusion effect did make contributions to ADC value in malignant and benign lesions. A higher f value was found in malignant tumors than that in benign lesions. The high perfusion fraction purported high vascularity in malignant tumors. So, the lower D value and higher f value strongly suggested a malignant lesion. Our results were in almost total agreement with the report by Sigmund et al. [21], but disagreed with Tamura et al. [27], who concluded no difference in any param-eters between benign and malignant tumors. Previous studies had demonstrated the usefulness of ADC value from monoexponential fitting in the differential diagnosis of breast lesions [8–16]. High perfusion fraction in malignant tumors influenced the DWI signal decay in opposite directions, so D value may be more useful in the differentiation between benign and cancerous tissues. Tissue microcirculation and cellularity contributions will influence ADC measurement in diametrically opposite directions. Therefore, Sig-mund et al. concluded that tissue diffusivity, by avoiding vascular contributions and marking cellularity more precisely, provided bet-ter differentiation of normal from malignant lesions than ADC. In the present study, we obtained the same results. While the AUC values for D and ADC were not significantly different, but D values still showed a higher AUC and specificity than those of ADC value. Because the perfusion effect could be avoided if monoexponential fit was performed using high b values (>200 s/mm2), just as we used in our study (b = 0 and 1000 s/mm2), perfusion may have a small contribution to ADC value, which lead to the similar results of D and ADC value. The f value in malignant tumors was statistically differ-ent from that in the others. As reported, f value was demonstrated as the signal intensity ratio of blood capillaries in tumor tissues [19]. Most studies showed f value was significantly increased in tumors [19], but Tamura et al. found no difference between malig-nant tumors and others. According to a study for prostate cancer [23], the apparent f value was sensitive to the range of b-values employed and their potential sampling of non-Gaussian effects. The f value was significantly increased in tumors with b-values below 750 s/mm2 and f became lower or indistinguishable from normal tissues with high b values. In Tamura’s study, b values were up to 3500 s/mm2, so no difference of f value was observed in malignant tumors and the others. In the present study, the AUC of f values in lesions was lower, about 0.723, it may be the fact that high b values of 800 and 1000 s/mm2 were used or maybe the perfusion effect was not obvious relative to tissue diffusion, but f values could further increased the diagnostic sensitivity and specificity.
D* was considered proportional to the mean capillary segment length and average blood velocity [29]. In the present study, malig-nant tumors showed a slightly slow blood velocity with a low D* values, but no difference was found in malignant tumors and benign lesions and the sensitivity and specificity for differentia-tion between benign and malignant lesions were the lowest. Our results were similar with other studies in renal lesions [30]. It may be related to the varying tumor vascularity among different tumor types.
One of the major limitations of our study was the biased small patient cohort with a small range of diseases types. A larger patient cohort with broader histological types of breast lesions might obscure the distinctions between benign and malignant groups. Secondly, the choice and appropriate number of b values suitable for breast IVIM are still unknown. Some biexponential studies in breast used 10 or 6 b values and 12 b values were used in this study. In one abdominal IVIM DWI study, only four fixed b values were used. So, the selection of b values and reduction in the number would then be an optimization procedure.
The bi-exponential IVIM model of DWI can be used to acquire both tissue diffusion parameters and perfusion microcirculation. The present study explained the perfusion and diffusion features of malignant tumors, benign lesions, simple cysts and normal breast tissues on the basis of the IVIM model by using multiple b values and showed their distinctive IVIM parameters features. A stepwise approach of these IVIM parameters effectively helped discriminat-ing malignant breast tumors from benign ones. The present results implied that IVIM imaging facilitated the understanding of the tis-sue characteristics of benign and malignant lesions as well as of normal breast tissues.
Conclusion
DWI response curves in malignant tumors, benign lesions andnormal fibroglandular tissues were found to be biexponential in comparison with the monoexponential fit in simple cysts. Com-
paring to DWI with monoexponential fit, IVIM provided separate quantitative measurement of D and f for cellularity and vascular-ity. Like ADC value, D also can be used to differentiate benign and
malignant lesions and had the highest specificity. Combining with f value, D value can increase diagnostic sensitivity and may have a vital role in screening breast MRI in high-risk women. Thus dif-
fusion imaging of solid breast lesions analyzed with biexponential model with multiple low and high b values can provide microen-vironment information, which could play an important role for
diagnosis, prognosis, and prediction of treatment response in patients with breast lesions without the use of exogenous contrastagent.
Conflict of interest
All of us and our institutions have no conflicts of interest, includ- ing any financial and personal relationships with other people or organizations that could inappropriately influence their work.
Acknowledgements
We gratefully acknowledge the assistance of Dr. Queenie Chan, from Philips Healthcare, Hong Kong, China, for support on IVIM methodology and for linguistic editing.Source of funding: The present study was supported by the National Scientific Foundation of China (No. 81271569 and 81271654) and Medical Scientific Research Foundation of Guang- dong Province, China (A2012040).
References
[1] Aberle DR, Chiles C, Gatsonis C, et al. Imaging and cancer: research strat- egy of the American College of Radiology Imaging Network. Radiology 2005;235(3):741–51.
[2] Leung JWT. Screening mammography reduces morbidity of breast cancer treat- ment. AJR Am J Roentgenol 2005;184(5):1508–9.
[3] Duffy SW, Smith RA, Gabe R, et al. Screening for breast cancer. Surg Oncol Clin N Am 2005;14(4):671–97.
[4] Peters NHGM, Borel Rinkes IHM, Zuithoff NPA, et al. Meta-analysis of MR imag- ing in the diagnosis of breast lesions. Radiology 2008;246(1):116–24.
[5] Kuhl CK. Concepts for differential diagnosis in breast MR imaging. Magn Reson Imaging Clin N Am 2006;14(3):305–28.
[6] Kul S, Cansu A, Alhan E, et al. Contribution of diffusion-weighted imaging to dynamic contrast-enhanced MRI in the characterization of breast tumors. AJR Am J Roentgenol 2011;196(1):210–7.
[7] Partridge SC, Demartini WB, Kurland BF, et al. Differential diagnosis of mam- mographically and clinically occult breast lesions on diffusion-weighted MRI. J Magn Reson Imaging JMRI 2010;31(3):562–70.
[8] Ei Khouli RH, Jacobs MA, Mezban SD, et al. Diffusion-weighted imaging improves the diagnostic accuracy of conventional 3.0-T breast MR imaging. Radiology 2010;256(1):64–73.
[9] Hirano M, Satake H, Ishigaki S, et al. Diffusion-weighted imaging of breast masses: comparison of diagnostic performance using various apparent diffu- sion coefficient parameters. AJR Am J Roentgenol 2012;198(3):717–22.
[10] Woodhams R, Matsunaga K, Iwabuchi K, et al. Diffusion-weighted imaging of malignant breast tumors: the usefulness of apparent diffusion coefficient (ADC) value and ADC map for the detection of malignant breast tumors and evaluation of cancer extension. J Comput Assist Tomogr 2005;29(5):644–9.
[11] Yabuuchi H, Matsuo Y, Okafuji T, et al. Enhanced mass on contrast-enhanced breast MR imaging: Lesion characterization using combination of dynamic contrast-enhanced and diffusion-weighted MR images. J Magn Reson Imaging JMRI 2008;28(5):1157–65.
[12] Yabuuchi H, Matsuo Y, Kamitani T, et al. Non-mass-like enhancement on contrast-enhanced breast MR imaging: lesion characterization using combi- nation of dynamic contrast-enhanced and diffusion-weighted MR images. Eur J Radiol 2010;75(1):e126–32.
[13] Rubesova E, Grell A-S, De Maertelaer V, et al. Quantitative diffusion imag- ing in breast cancer: a clinical prospective study. J Magn Reson Imaging JMRI 2006;24(2):319–24.
[14] Marini C, Iacconi C, Giannelli M, et al. Quantitative diffusion-weighted MR imaging in the differential diagnosis of breast lesion. Eur Radiol 2007;17(10):2646–55.
[15] Chen X, Li W, Zhang Y, et al. Meta-analysis of quantitative diffusion-weighted MR imaging in the differential diagnosis of breast lesions. BMC Cancer 2010;10:693.
[16] Mazaheri Y, Afaq A, Rowe DB, et al. Diffusion-weighted magnetic resonance imaging of the prostate: improved robustness with stretched exponential mod- eling. J Comput Assist Tomogr 2012;36(6):695–703.
[17] Le Bihan D, Breton E, Lallemand D, et al. MR imaging of intravoxel incoher- ent motions: application to diffusion and perfusion in neurologic disorders. Radiology 1986;161(2):401–7.
[18] Andreou A, Koh DM, Collins DJ, et al. Measurement reproducibility of perfusion fraction and pseudodiffusion coefficient derived by intravoxel incoherent motion diffusion-weighted MR imaging in normal liver and metastases. Eur Radiol 2013;23(2):428–34.
[19] Sumi M, Van Cauteren M, Sumi T, et al. Salivary gland tumors: use of intravoxel incoherent motion MR imaging for assessment of diffusion and perfusion for the differentiation of benign from malignant tumors. Radiology 2012;263(3):770–7.
[20] Eckerbom P, Hansell P, Bjerner T, et al. Intravoxel incoherent motion MR imag- ing of the kidney: pilot study. Adv Exp Med Biol 2013;765:55–8.
[21] Sigmund EE, Cho GY, Kim S, et al. Intravoxel incoherent motion imag- ing of tumor microenvironment in locally advanced breast cancer. Magn Reson Med Off J Soc Magn Reson Med Soc Magn Reson Med 2011;65(5): 1437–47.
[22] Le Bihan D, Turner R, MacFall JR. Effects of intravoxel incoherent motions (IVIM) in steady-state free precession (SSFP) imaging: application to molecular diffu- sion imaging. Magn Reson Med Off J Soc Magn Reson Med Soc Magn Reson Med 1989;10(3):324–37.
[23] Pang Y, Turkbey B, Bernardo M, et al. Intravoxel incoherent motion MR imaging for prostate cancer: an evaluation of perfusion fraction and diffusion coefficient derived from different b-value combinations. Magn Reson Med Off J Soc Magn Reson Med Soc Magn Reson Med 2013;69(2):553–62.
[24] Delille J-P, Slanetz PJ, Yeh ED, Kopans DB, Garrido L. Breast cancer: regional blood flow and blood volume measured with magnetic susceptibility-based MR imaging—initial results. Radiology 2002;223(2):558–65.
[25] Jansen SA, Lin VC, Giger ML, et al. Normal parenchymal enhancement patterns in women undergoing MR screening of the breast. Eur Radiol 2011;21(7):1374–82.
[26] DeMartini WB, Liu F, Peacock S, et al. Background parenchymal enhance- ment on breast MRI: impact on diagnostic performance. AJR Am J Roentgenol 2012;198(4):W373–80.
[27] Tamura T, Usui S, Murakami S, et al. Biexponential signal attenuation analysis of diffusion-weighted imaging of breast. Magn Reson Med Sci MRMS Off J Jpn Soc Magn Reson Med 2010;9(4):195–207.
[28] Baron P, Dorrius MD, Kappert P, Oudkerk M, Sijens PE. Diffusion-weighted imaging of normal fibroglandular breast tissue: influence of microperfusion and fat suppression technique on the apparent diffusion coefficient. NMR Biomed 2010;23(4):399–405.
[29] Le Bihan D, Breton E, Lallemand D, et al. Separation of diffusion and per- fusion in intravoxel incoherent motion MR imaging. Radiology 1988;168(2): 497–505.
[30] Chandarana H, Lee VS, Hecht E, Taouli B, Sigmund EE. Comparison of biexponen- tial and monoexponential model of diffusion weighted imaging in evaluation of renal lesions: preliminary experience. Invest Radiol 2011;46(5):285–91.